Home > NF2 Facts & Information >
Eyes and Vision Issues
Last Updated: 05/8/26
NF2 Eye Issues
- Cataracts -
Juvenile Cataracts (PSC) - Retinal Detachment
- Damage to Eye Nerves -
cranial nerves 2, 3, 4, and 6 - Papilledema
(optic disc edema) - Ocular Migraine (retinal migraine)
- Retinitis Pigmentosa (RP)
(retinal degeneration) - Combined Hamartoma of the
Retina and RPE - Retinal Microaneurysms
- Epiretinal Membrane
- Conjunctivitis
(eye cold) - Physiopedia
(severe dry eyes) - Nystagmus - oscillopsia
(ocular flutter)cross) - Diplopia (double vision)
- Gaze-evoked Tinnitus (GET)
NF1 Eye Issues
- Congenital Glaucoma
- Lisch Nodules
- Optic Nerve Gliomas
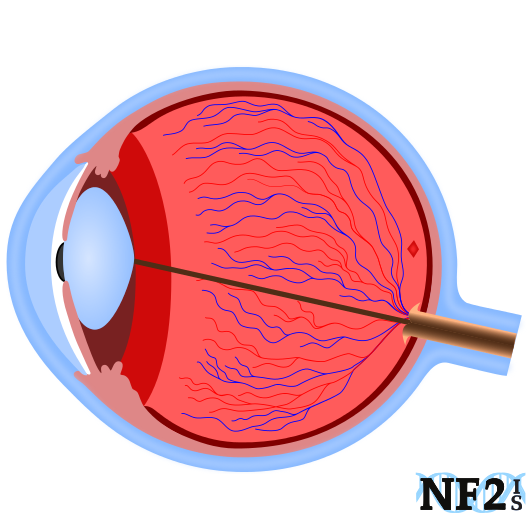
Everyone with Neurofibromatosis (NF) NF1, and NF2 - SWN should see a Neuro-ophthalmologist who is familiar with NF yearly for optic neurological issues that can develop.
A neuro-ophthalmologist is a physician (neurologist or ophthalmologist) specializing in diseases affecting Vision that originate from the nervous system. It is not that an ophthalmologist would not be familiar enough with some of the neurological issues that result from NF, but tests that need to be done and reviewed require seeing a Neuro-Ophthalmologist, including, but not limited to, the review of actual MRI scans.
What to bring for an Eye exam:[5]
- Your glasses or contacts and a copy of your prescription if you have it.
- YInclude information stating the specific reason for the visit and a list of existing eye issues
- YA list of medications, especially eye-related
- YAny relevant prior medical records, including radiology reports
- YA recent CD of an MRI of the brain so the doctor can review the images.
The NF2 condition is rare; the rare condition includes tumors and rare eye problems. The eye problems are uncommon enough that twenty-percent (20%) of vision loss of individuals with NF2 with a diagnosis of ocular abnormalities. Also, some eye abnormalities, including juvenile cataracts, are used as a part of the NF2 diagnosis criteria to diagnose individuals early.
Common eye problems individuals with NF2 may face include:
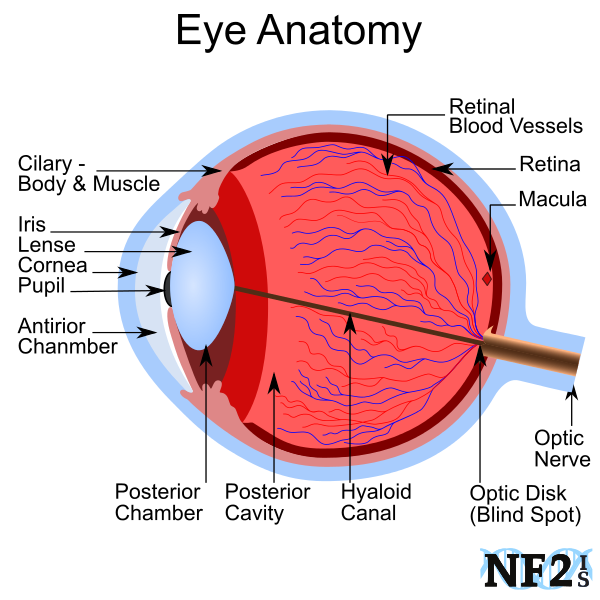
- Cataracts - juvenile cataracts (PSC)
- Retinal Detachment
- Damage to Eye Nerves - cranial nerves 2, 3, 4, and 6
- Papilledema (optic disc edema)
- Ocular Migraine (retinal migraine)
- Retinitis Pigmentosa (RP) (retinal degeneration)
- Combined Hamartoma of the Retina and RPE
- Retinal Microaneurysms
- Epiretinal Membrane
- Viral Conjunctivitis (eye cold)
- Physiopedia (severe dry eyes)
- Nystagmus - oscillopsia (ocular flutter)
- Diplopia (double vision)
- Gaze-evoked Tinnitus (GET)
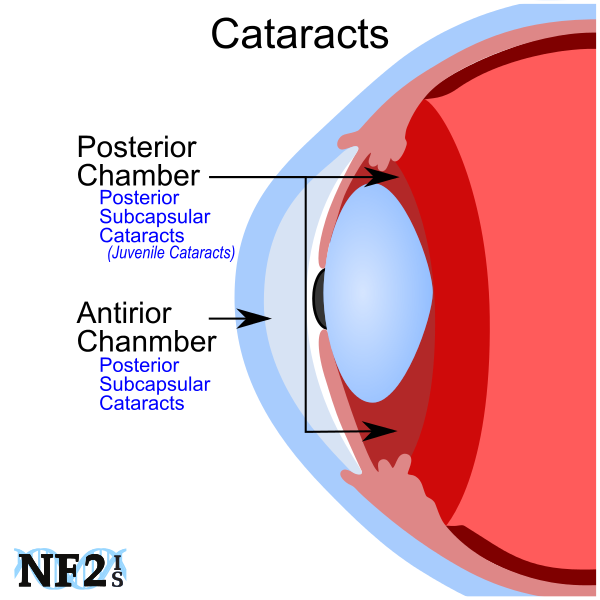
1. Cataracts - Juvenile Cataracts (PSC)
Juvenile cataracts occur in approximately 90% of NF2. Also known as; posterior subcapsular, capsular cataracts, or PSC cataracts. Individuals with NF2 often start to develop juvenile cataracts at or shortly after birth and is one of the simplest ways to determine early if an individual may have NF2 like other family members.
While individuals with NF2 can potentially develop age-related cataracts like any other person, there is a high risk of juvenile cataracts. When age-related cataracts develop in people in general, it would develop by 65 years of age but can develop in individuals as young as 40. However, individuals who have NF2 and develop Juvenile Cataracts, it is a Secondary Form of Cataracts that can develop at birth, or would develop well before 65 years.
The formation of NF2 cataracts is typically PSC cataracts, posterior subcapsular lens opacities, which can cause complications in surgical treatment. Individuals with NF2 sometimes develop CC cataracts.
Juvenile Cataracts can result in visual impairments including; blurry vision, poor vision at night, severe reactions to glare, as well as a visibly cloudy or white spot that can be seen covering the eye.
1. Posterior Subcapsular/Capsular Cataracts / PSC Cataracts / Juvenile Cataracts
Posterior subcapsular/capsular cataracts (PSC Cataracts) is a form of cataract that forms behind the iris and lenses in the posterior chamber.
PSC visual disturbance is a halo effect or glare around lights.
2. Cortical Cataracts (CC)
Cortical cataracts (CC), peripheral Cortical Lens Opacities or simply Cortical Opacities, is a form of Cataracts that occurs just behind the Cornea inside the Anterior Chamber of the eye.
CC visual disturbance that would result from this include; peripheral vision (outer vision) issues, at the edges of the lens of the eye as well as blurred vision, glare, contrast, and depth perception issues.
Cataract Treatment
Surgical options are available for both Cataract forms, typically requires artificial lens "intraocular lens" implantation at the time of cataract surgery to replace the damaged natural lens also known as "crystalline lens." Following Cataract surgery glasses will likely be needed, Following Cataract surgery glasses will likely be needed, or will require a change in prescription.
Surgical Issue
Retinal Detachment is a possible issue, following cataract surgery. In prevention of complications that could result in permanent blindness, quick response following symptoms of retinal detachment is important. Make certain the surgeon is trained in and has treated people with PSC cataracts in the past.
Increased Risk Factors for Cataract development
In addition to age, other factors may increase the risk of cataract development. These include; diabetes, smoking, overexposure to sunlight, and certain medications, such as steroids."
Radiation Treatments- Cataracts are common side effects of total body radiation treatments.
http://umm.edu/health/medical/reports/articles/cataracts2. Retinal Detachment
Retinal detachment (retinal tear) is the result of a weak or thin retina which detaches leaving a break in the retinal thereby allowing fluid to pass under the retina. Following this, the retina peels away from the back of the eye. With this issue, the retina separates from the underlying tissue resulting in vision loss and blindness.
"Rhegmatogenous retinal detachment (RRD) is the most common form of retinal detachment, where a retinal 'break' allows the ingress of fluid from the vitreous cavity to the subretinal space, resulting in retinal separation." [Steel, David (2014)]
"
Causes
Retinal Detachment is typically the result of Cataract surgery weeks or months later, but can also be Spontaneous as well.
Signs
Warning signs include flashing lights, floaters, or blind spots.
Treatment
Surgical options are possible to correct this if done within twenty-four hours (24-hours) after detachment occurs.
3. Cranial Nerves of the Eye
(cranial nerve 2, cranial nerve 3, cranial nerve 4, and cranial nerve 6)
There are 12 pairs of nerves in the central nervous system, a left and a right nerve for each nerve type. Some control muscles and others control senses. The visual processing center of the brain is the occipital lobe with different areas of the lobe affecting different areas in the visual field.
Four Cranial Nerve pairs control the eyes themselves, including; the Optic Nerve, the Oculomotor Nerve, the Trochlear Nerve and the Abducens Nerve.
- Cranial Nerve 2 (CN II) - Optic Nerve: Vision
- Cranial Nerve 3 (CN III) - Oculomotor Nerve: Muscles for the Eye
- Levator Palpebrae Superioris Muscle: this muscle keeps the eyelids open
- Constriction of the Pupils: light sensitivity, adaption to the change in light; dark to bright, or bright to dark.
- Cranial Nerve 4 (CN IV) - Trochlear Nerve: Muscles for Eye Movement
- Cranial Nerve 6 (CN VI) - Abducens Nerve: Eye Movement
CNII (Cranial Nerve 2), carries Vision to the brain. This nerve does not contain Schwann cells.
CN3, (Cranial Nerve 3) has two functions it controls:
CN IV (Cranial Nerve 4), controls eyeball movement, rotating, up, down, left and right.
Lateral Rectus Muscle: lateral vision - left to right
4. Papilledema (optic disc edema)
Papilledema is an issue where swelling or pressure on the optic disc (entry point of the optic nerve to the back of the eye) results in different intervals of loss and regaining vision. If papilledema is left untreated, it can permanent loss of vision.
This issue can be seen in an eye exam as the pressure behind the eye or eyes and is typically the result of intracranial pressure (obstructive hydrocephalus) from tumor masses in the brain. Left untreated papilledema can result in permanent blindness if the reason for the pressure increases.
This condition is best identified following a head MRI and exam by a neuro-ophthalmologist.
Symptoms:
Symptoms include; unexplained nausea, straining, coughing, bending, or ocular migraines. Symptoms may also be worse when changing position, including movement from either resting flat to sitting or standing after sitting.
Tip:
A slower change of position will help minimize dizziness and visual disturbances.
Diagnostic Tests:
Diagnosis of papilledema requires; 1) a brain MRI, and 2) visual field test for points of missing vision in eyes. Papilledema can lead to permanent blindness as well as RPE pigmentary changes. Testing may also include a fluorescein angiography to show the grade of papilledema.
Management:
Different treatments may be necessary but managed initially with either; prescription medication or surgery to remove the tumor cause of the pressure. It is also possible that the papilledema could have been the result of medication and can be corrected with dose change.
5. Ocular Migraines (retinal migraines)
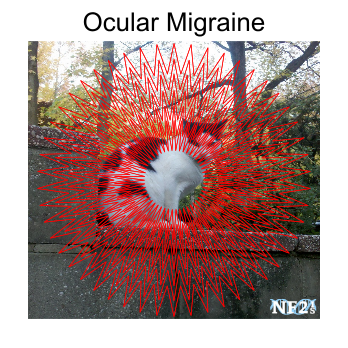
Neurofibromatosis Type 2 (NF2) can easily result in different forms of headache types, superficially two different migraine types including; 1) vestibular migraines, and 2) ocular migraines. Contact doctors on the first occurrence of either type. Both migraine types are signs of serious health issues
Symptom: Ocular migraines (retinal migraines) can include a temporary blind spot, temporary blurring of vision, or vision loss is usually bilateral for different periods of time.
Reason: Ocular migraines are a common occurrence with swelling in the brain and papilledema. Not all occurrences of an ocular migraine require medical management, but episodes should be discussed with doctors since it could be a sign of a serious health issue.
Treatment: Aspirin, caffeine, or medication slow release of aspirin and caffeine. However, water may also help since migraines can also be the result of excess caffeine can trigger migraines of any sort. Prescription options may also help.
6. Retinitis Pigmentosa (RP) and Retinal Degeneration
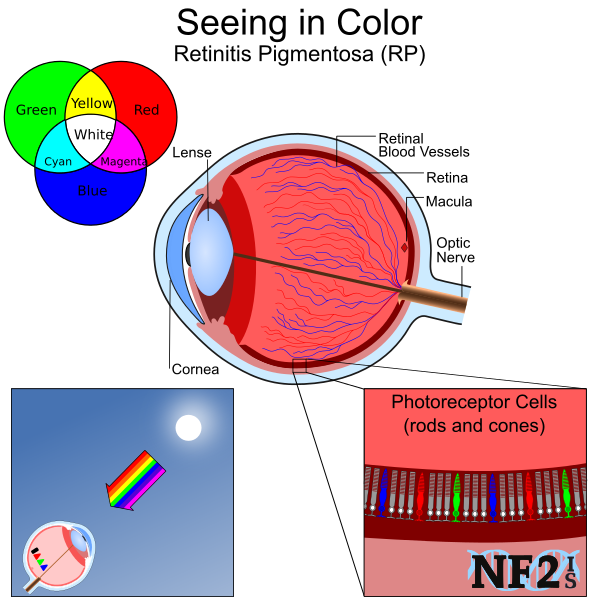
Retinitis pigmentosa (RP) is a name used for conditions that can cause retinal degeneration, vision loss. Pigmentosa is a layer of cells in the back wall of the eye necessary to process light and differentiate color for the optic nerve. RP can result in central vision loss that may eventually result in peripheral vision loss. Central vision is a sight in the center view of the eye. Peripheral vision is the outer range of vision.
Other names for RP include; 1) hyperpigmentation RPE; 2) hyperpigmentation of the retinal pigment epithelium, 3) pigmented layer of the retina, 4) pigmentum nigrum, or 5) intra-retinal leakage of fluorescein.
Retinal pigment epithelium (RPE) (pigmented layer of the retina) is a layer in the eye that shields the retina from excess incoming light.
Possible Options
ClinicalTrials.gov
"CB-PRP in Retinitis Pigmentosa (SiCord)" Stem Cell Treatment - Trial Start date November 2020
Subretinal injection of umbilical cord blood platelet-rich plasma (CB-PRP)
SecondSight. Argus II. "The First Bionic Eye" Retinal Prosthesis System (April 2018)
7. Combined Hamartoma of the Retina and Retinal Pigment Epithelium (CHRRPE or CHRPE)
A condition called combined hamartoma of the retina and retinal pigment epithelium (CHRRPE or CHRPE), is when glial tissue in different parts of the eye. CHRPE causes blood vessels issues and pigment epithelium, resulting in profound vision loss.
Combined hamartoma of the retina and the retinal pigment epithelium is a rare benign lesion in the macula. Juxtapapillary on peripheral location is common in children and that consists of the glial cells (vascular tissue), and sheets of pigment epithelial cells.
Hamartoma, pigmented benign cell tissue, an excess of normal tissue. Hamartoma of the retina is also known as retinal hamartoma.
Juxtapapillary: choroidal neovascular membrane following optic neuritis.
8. Retinal Microaneurysms
Retinal microaneurysms are a small aneurysm in retinal capillaries; small amounts of swelling in the wall of blood vessels within the eye that look like small, round, red spots.
9. Epiretinal Membrane
Epiretinal membrane is a buildup of scar tissue that covers the retina.
A gel that naturally forms over the lens and pupil of the eye called the "the vitreous" is a result of an immune system response to protect the retina. Scar-like cells make up this gel, are a form of scar tissue that can form over the eye and damage the retina's surface. As it gets thicker if it does not sit as a flat layer, it puckers, and the film causes blurry, distorted vision.
Epiretinal membrane is typically the result of either; 1) posterior vitreous detachment (PVD) or 2) diplopia (double vision).
Synonyms for epiretinal membrane include; 1) macular pucker, 2) cellophane maculopathy, 3) retina wrinkle, 4) surface wrinkling retinopathy, 5) premacular fibrosis, and 6) internal limiting membrane disease.
10. Conjunctivitis (eye cold)
When the eye closes the eyelid flushes the eye with a tear to wash away bacteria. When the eye is exposed to all of the bacteria the eye encountered, or the eye does not produce enough fluid to wash the eye when the eye closes, the individual may develop an eye infection, the eye infection is commonly called simply pink eye with or without mucus discharge in the eye and exterior, with medical term of conjunctivitis.
For individuals with NF2, viral conjunctivitis is common but is the result of the inability of the eye producing tears, fluid, or enough tears to protect the eye. The problem is result of tumor growth damage to the facial nerve, cranial nerve 7 (CN7).
Issues with conjunctivitis may start several years or longer before other parts of the facial nerve may suffer from other complications.
Treatment: Talk to regular physician about antibacterial eye drops.
11. Physiopedia (Severe Dry Eyes)
Severe dry eyes for individuals with NF2 can be the result of different issues, development of severe dry eyes in individuals with NF2 is most commonly the result of either; 1) vestibular schwannoma, or acoustic neuroma growth and nerve damage, 2) damage to cranial nerve 7 (facial nerve), 3) damage to cranial nerve 5 (trigeminal nerve), or 3) tumor-drug treatments.
Dry Eyes and tumor-drug treatments:
Many of the tumor suppressor drug treatents including; Bevacizumab (Avastin™), Lapatinib (Tykerb™) and RAD 001 - Everolimus (Afinitor™). These medications can cause dry eye issues and require excessive individuals to drink more water to compensate.
Dry eye issues a result of Avastin, typically only results for the first three (3) months of treatment. When the dry eye is the result of medication, dry eye issues usually stop with breaks or when discontinuing the medication.
Facial Nerve or Trigeminal Nerve Damage:
If dry eyes are an issue, it could mean that the weakening of either the facial nerve (CN7) or the result of the trigeminal nerve (CN5).
The facial nerve, cranial nerve 7, affects the muscles that open and close the eye in addition to producing fluid to keep moisture in the eye. Keeping moisture in the eyes is important to prevent other issues like cracked cornea.
The trigeminal nerve, cranial nerve 5, controls the function of the sensation of different parts of the face and some movements of the head; jaw and nasal cavity.
12. Nystagmus - oscillopsia (ocular flutter)

Nystagmus causes ocular flutter. Ocular flutter is a random movement of eyes away from the point of intended focus and often results in reduced vision. If ocular flutter either gets worse, or nothing is done to manage the movement of the eye, it can lead to oscillopsia.
Oscillopsia can be either mild blurring or rapid and periodic jumping of vision. Oscillopsia is a visual disturbance in which objects in the visual field appear to oscillate. The severity of the effect may range from a mild blurring to rapid and periodic jumping. The development of Nystagmus is common for individuals with NF2; it can be the result of the following issues:
- Congenital Nystagmus (Infantile Nystagmus): Congenital nystagmus sometimes is the result of juvenile cataracts.
- Vestibular Nystagmus: A result of damage to the vestibular system, or vestibular nerve tumors.
Oscillopsia is an incapacitating condition experienced by many patients with neurological disorders.
13. Diplopia (double vision)
Diplopia (double vision) is a common issue for people with NF2. Prism glasses might be options to correct these issues if noticed early enough. Depending on the reason for the double vision surgery may be an option.

I. Forms of Diplopia
Temporary
Binocular
Monocular
Voluntary
Temporary diplopia might result in binocular and monocular vision and can be the result of; head trauma, certain medications, alcohol, or eye strain. Temporary Diplopia can result in permanent diplopia.
Binocular diplopia is misalignment with two (2) eyes: both eyes facing in, booth facing out, one eye facing in, or one facing out when seeing double vision.
Binocular diplopia is the result of strabismus. There is two form of strabismus; cross-eye and walleye, binocular diplopia, are different angles of perception and can be the result of eye muscle coordination or a brain issue.
Muscle coordination could be the result of damage to cranial nerves 3, 4, or 6; frequently the result of tumor damage, which can be fixed with surgery to remove the tumor and tightening of the weakened muscles.
Amblyopia is a brain issue that results in one lazy eye that has no vision of perceived vision in the other eye. Cross-eye and walleye treated early can prevent the development of Amblyopia.
Monocular diplopia is damage to an eye that results in the double vision seen with only the damaged eye. Monocular diplopia is the result of damage to the cornea of the eye itself and results in multiple images, seen.
Voluntary diplopia is when an individual has normal eye alignment but can switch to Binocular eye alignment or Binocular eye alignment and can switch to normal eye alignment.
II. Result of
Many issues can result in diplopia, some of which include:
Cornea Scars
Juvenile Cataracts
Eye Muscle Issues
Eye Cranial Nerve Damage
Cornea scars and dry cornea can damage the eye and result in double vision. Dry eyes are a common NF2 issue, and many individuals need to use a constant amount of eye drops.
Juvenile cataracts frequently develop at a very early age for individuals with NF2 and would result in distorted vision.
If the muscle in one of the eyes is weaker than the other, the development of double vision would be the result of the eyes not focusing together.
Eye muscle issues might develop from damage to the facial nerve from of eyelid closure issues.
The third, fourth, and sixth cranial nerves each control different aspects of eye muscle position. Diplopia could be the result of damage to CN3 the oculomotor nerve, CN4 the trochlear nerve or CN6 the abducens nerve.
III. Management
Management of diplopia can be possible with the following options:
Eye Exercise
Visit a Physical Therapist to learn the best eye exercise therapy.Lazy Eye Glasses:
Prism EyeglassesEye Patch:
It can help to wear a patch over the good eye to encourage the strengthening of the muscle of the weaker eye.Surgery (Strabismus Muscle Surgery):
Due to surgical stress individuals with NF2 are often told by doctors not to undergo surgery to correct this since other options are available.
14. Gaze-evoked Tinnitus (GET)
Gaze-evoked tinnitus (GET) is a form of Tinnitus sub-form of a class of tinnitus called somatosensory tinnitus; is affected by either; horizontal, or vertical, not necessarily both. Eye movements affect pitch and tone heard. Eye movements affect pitch and tone heard.
The development of GET is one of the results of damage to hearing. GET can occur after removal of vestibular schwannoma (VS) or acoustic neuroma (AN), which damages cranial nerve 8, associated with the hearing and balance nerves. GET can start after VS damage in one side of the head and seem to be a sound into that ear when the eyes move. When VS damage occurs in both ears, also known as bilateral damage; the sound might be in one or both ears, when the eyes move.
It is unknown exactly why this form of Tinnitus occurs, since it does not always occur after removal of VS, but it is believed to be the result of the brains attempts to find sound.
15. Sources
-
Kang, H. M., Koh, H. J., & Chung, E. J. . "Spectral-domain Optical Coherence Tomography of Combined Hamartoma of the
Retina and Retinal Pigment Epithelium in Neurofibromatosis." Korean Journal of Ophthalmology, 27(1), 68-71. (2013)
Source: http://synapse.koreamed.org/search.php?where=aview&id=10.3341/kjo.2013.27.1.68&code=0065KJO&vmode=FULL | DOI: doi.org/10.3341/kjo.2013.27.1.68 -
Feucht M, Kluwe L, Mautner V, Richard G. Feucht, Matthias, et al.
"Correlation of nonsense and frameshift mutations with severity of retinal abnormalities in neurofibromatosis 2."
Archives of Ophthalmology 126.10 (2008): 1376.
Source: http://archopht.jamanetwork.com/article.aspx?articleid=420813 | DOI: doi:10.1001/archopht.126.10.1376 -
Rachitskaya, Aleksandra. "Combined Hamartoma of Retina and Retinal Pigment Epithelium" EyeWiki. The American Academy of Opthalmology. (2015)
Source: http://eyewiki.aao.org/Combined_Hamartoma_of_Retina_and_Retinal_Pigment_Epithelium -
Wells, Jill R. et al. EyeNet. "Diagnosing and Treating Neurotrophic Keratopathy," The American Academy of Opthalmology. (2008)
Source: https://www.aao.org/eyenet/article/diagnosing-treating-neurotrophic-keratopathy?julyaugust-2008 -
Harada, Takayuki, et al. "Severe optic disc edema without hydrocephalus in neurofibromatosis 2."
Hokkaido University School of Medicine. Japanese Ophthalmological Society. 42.5 (1998): 381-384.
Source: http://www.nichigan.or.jp/jjo-oj/pdf/04205/042050381.pdf -
Sanchez, T. G., & Rocha, C. B. "Diagnosis and management of somatosensory tinnitus: review article." Clinics, 66(6), 1089-1094. (2011)
Source: http://www.scielo.br/scielo.php?pid=S1807-59322011000600028&script=sci_arttext | DOI: http://dx.doi.org/10.1590/S1807-59322011000600028 -
National Institutes of Health (NIH).
"Omega-3 Fatty Acids Protect Eyes Against Retinopathy, Study Finds."
NIH News. National Eye Institute., 1:00 p.m. EDT. (2007)
http://www.nih.gov/news/pr/jun2007/nei-24.htm -
Weill Cornell Medical College. "Neuro-ophthalmology." (Document Retrieved: Jun2 2014.)
http://weillcornelleye.org/services/neuro.html - Discovery Eye. "What Is Retinitis Pigmentosa?" http://discoveryeye.org/what-is-retinitis-pigmentosa/
-
Osborne, Jonathan Robert. "The Differential Diagnosis of Meniere's Disease and Vestibular Migraine" UC Research Repository.
Department of Communication Disorders. (2017)
Source: https://ir.canterbury.ac.nz/bitstream/handle/10092/13438/MAud%20thesis%20-%20Jon%20Osborne.pdf -
Crandall E. Peeler, MD, Jane C. Edmond, MD, et al. "Visual and ocular motor outcomes in children with posterior fossa tumors"
Journal of American Association for Pediatric Ophthalmology and Strabismus (JAAPOS). Vol. 21, Issue 1 (September 2017)
Source: http://www.jaapos.org/article/S1091-8531(17)30213-6/fulltext DOI: 10.1016/j.jaapos.2017.05.032 -
Eye Wiki. "Papilledema." (Reviiwed: 10/08/19)
http://eyewiki.aao.org/Papilledema -
Hereditary Ocular Disease "Neurofibromatosis Type 2 (NF2)."
A href="http://disorders.eyes.arizona.edu/category/genes/nf2" target="_blank">http://disorders.eyes.arizona.edu/category/genes/nf2 -
NF Center. "NF1 optic pathway glioma."
https://nfcenter.wustl.edu/research/laboratory-research/nf1-optic-pathway-glioma-other-brain-tumor-research/ - Kumar, Vinay, et al. "Robbins and Cotran pathologic basis of disease." (2005).
-
Eva Duchnowski OD "Juxtapapillary choroidal neovascular membrane following optic neuritis" (2010)
https://onlinelibrary.wiley.com/doi/full/10.1111/j.1444-0938.2009.00440.x | DOI: https://doi.org/10.1111/j.1444-0938.2009.00440.x -
Destro, Maryanna, et al. "Retinal manifestations of neurofibromatosis: diagnosis and management." Archives of ophthalmology 109.5 (1991): 662-666.
Link: https://jamanetwork.com/journals/jamaophthalmology/article-abstract/639066 | DOI: doi:10.1001/archopht.1991.01080050076033 -
Kaye, Laurence D., et al. "Ocular findings associated with neurofibromatosis type II." Ophthalmology 99.9 (1992): 1424-1429.
Link: https://www.sciencedirect.com/science/article/pii/S0161642092317890 | DOI: https://www.aaojournal.org/article/S0161-6420(92)31789-0/pdf -
Alkatan, Hind M., Sawsan S. Bakry, and Mohammad A. Alabduljabbar. "Ocular Findings in Neurofibromatosis."
Neurofibromatosis-Current Trends and Future Directions. IntechOpen, 2019.
Source: https://www.intechopen.com/online-first/ocular-findings-in-neurofibromatosis | DOI: 10.5772/intechopen.90021


 |Google Play
|Google Play